2026 Vol. 8, No. 13
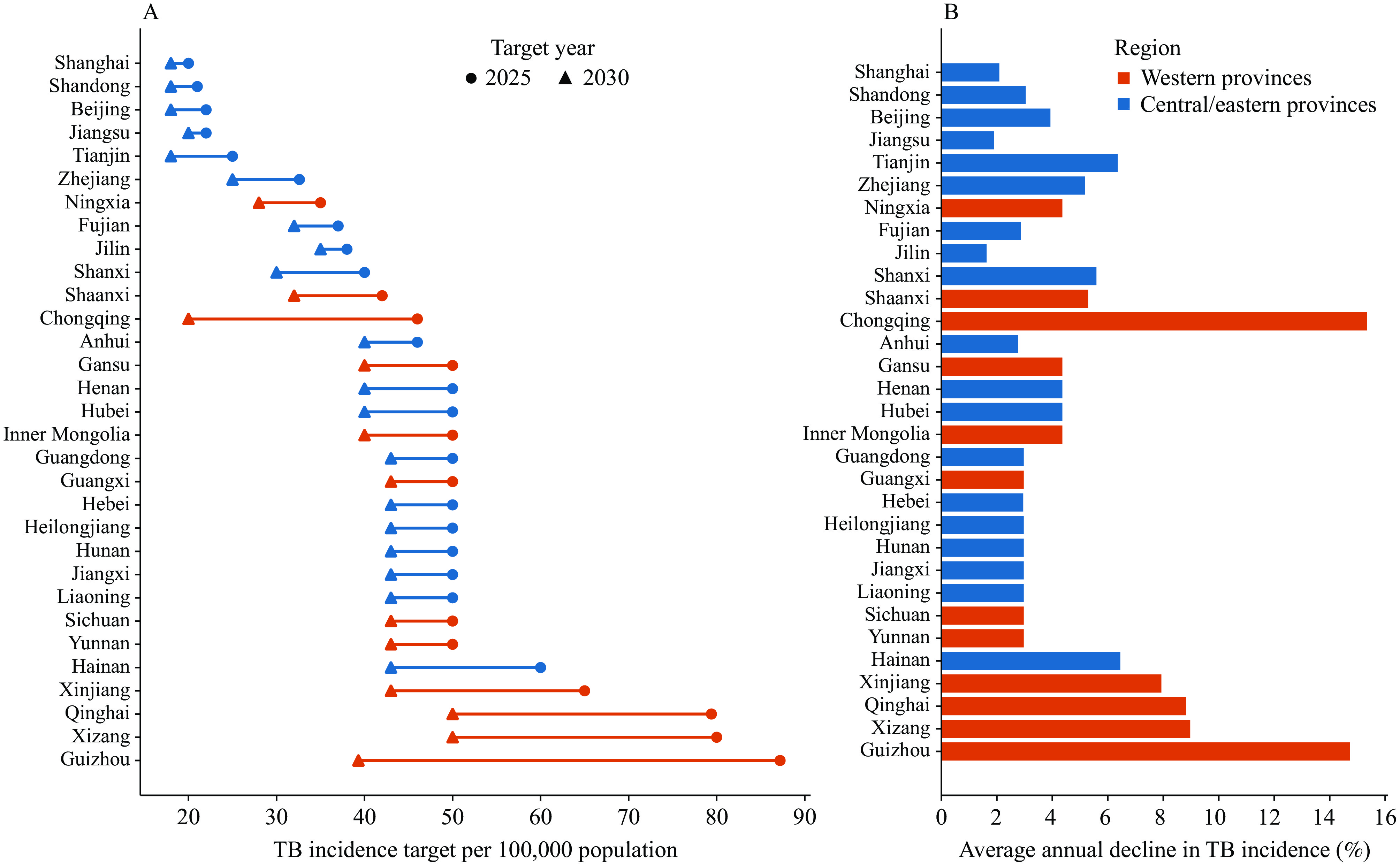
The global trajectory for tuberculosis (TB) elimination remains precarious, characterized by a recent but fragile and insufficient decline in its incidence by 2024, the first since the coronavirus disease 2019 (COVID-19) pandemic. Progress is severely hampered by the failure to meet the ambitious 2025 End TB targets and is further threatened by anticipated funding cuts, necessitating a translation of widely accepted concepts of “high-level multi-sectoral cooperation” and “strict accountability” to concrete solutions. In contrast, China has achieved remarkable progress, meeting its goal of a 20% reduction in TB incidence from 2015 to 2024, suggesting a transition toward a lower-incidence setting. This success reflects a deliberate, science-driven, and strategic transformation. In this Personal View, we describe China’s clearly defined national and provincial TB incidence-reduction targets for 2025 and 2030, as well as its comprehensive TB control program spanning the full continuum of care. China’s integrated strategy, combining political commitment, rigorous strategy, sustainable financing, empowering research and innovation, the zoonotic and anthroponotic TB approach, and strong accountability mechanisms, offers a blueprint for low- and middle-income countries. It outlines a specific implementation pathway to revitalize global efforts to combat TB and restore confidence in the feasibility of ending TB.
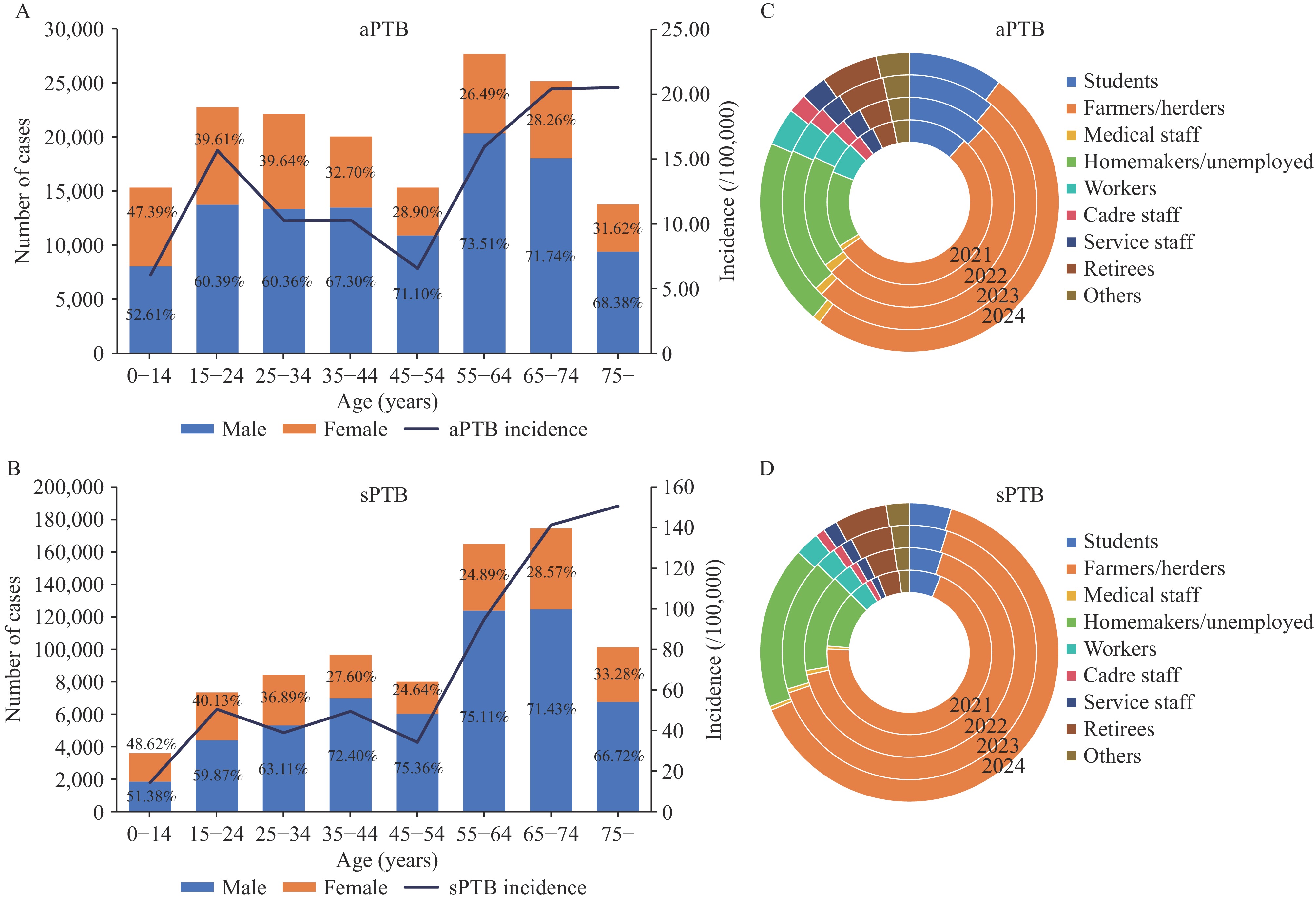
Tuberculosis (TB) remains a major public health challenge in China, which ranks fourth among the 30 high-burden countries worldwide. Individuals with asymptomatic Pulmonary TB (aPTB) may act as “silent transmitters”, contributing to undetected community transmission and hindering progress toward the End-TB goals. This study examined the epidemiological characteristics of patients with aPTB in China from 2021 to 2024 to inform targeted control strategies.
Data were obtained from the China Information System for Disease Control and Prevention for the period 2021–2024 and included TB cases with complete symptom records. aPTB was defined as cases without recorded cough symptoms, whereas symptomatic TB was defined as cases with recorded cough symptoms. Descriptive statistical analyses compared the demographic, clinical, and healthcare-seeking characteristics of patients with aPTB and symptomatic TB.
Among 973,299 PTB cases with complete symptom records, 16.66% were classified as aPTB. This proportion remained relatively stable throughout the study period, with a slight peak observed in 2022. Higher proportions of aPTB were observed among individuals aged 55–64 years (17.07%), 65–74 years (15.51%), and 15–24 years (14.03%), and among farmers and herders (50.87%). A mild seasonal trend was observed. Geographically, high-incidence areas were concentrated in western and southwestern China.
aPTB constitutes a substantial component of the total TB burden in China. Strengthening active case detection in high-risk populations, optimizing medical resources in western China, and integrating aPTB control programs into national prevention and control plans for TB to mitigate hidden transmissions and advance national End-TB objectives.
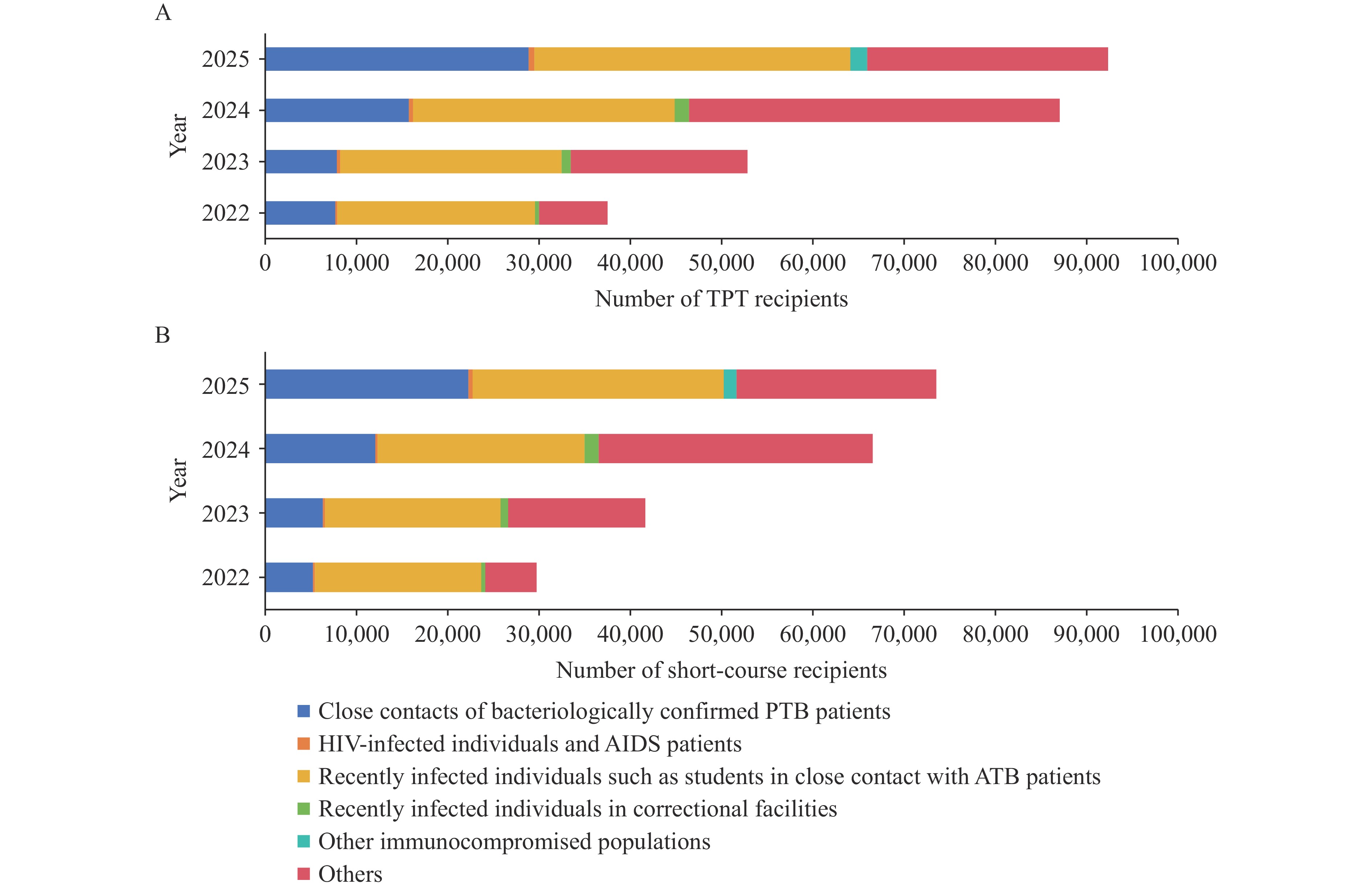
Tuberculosis preventive treatment (TPT) is critical in preventing latent tuberculosis infection (LTBI) progression to active tuberculosis. China has integrated TPT into national Tuberculosis (TB) control; however, systematic national data on TPT implementation in China are scarce.
TPT recipient number in China increased 2.5-fold (2022–2025), with around 79% using short-course regimens. Among 2,676 individuals with LTBI, TPT acceptance and completion rates were 45.14% and 85.18%, respectively. Key acceptance factors included age, ethnicity, occupation, treatment institution, immunocompromised status, and purified protein derivative results.
To improve TPT effectiveness, public health strategies should integrate TPT into routine clinics, promote short-course regimens, and target high-risk groups (e.g., immunocompromised individuals and the elderly) to increase acceptance rates and reduce disparities to achieve TB elimination.
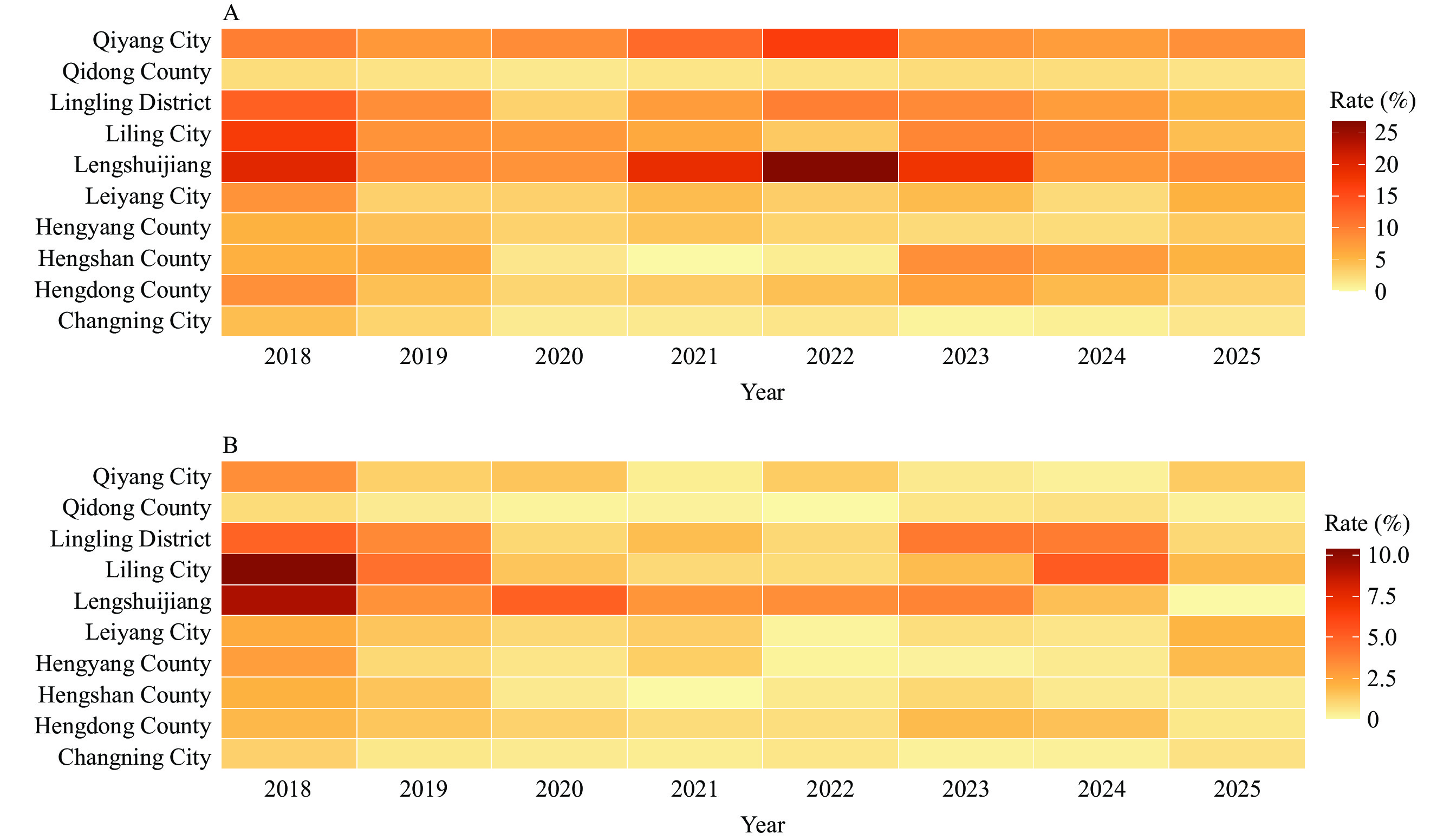
Tuberculosis (TB) is a deadly global infectious disease, and China has a high burden of rifampicin-resistant (RR) and multidrug-resistant (MDR) TB, according to the World Health Organization. Prior treatment, Regional disparities, demographics (age/sex), and comorbidities (e.g., diabetes) are associated with an elevated risk of drug-resistant TB.
We analyzed 25,978 bacteriologically confirmed pulmonary TB (PTB) cases in 10 sites in Hunan Province and found lower first-line drug resistance rates than national/provincial estimates (2018–2025). Retreatment, age 25–44 years, diabetes, and Lengshuitan residence were independent predictors of resistance. Resistance declined during the pandemic, rebounded slightly thereafter, and displayed a 4.0% annual decrease (statistically significant). There was notable inter-county heterogeneity (intraclass correlation coefficient=0.11). Hunan shifted to molecular testing (82.79% of susceptibility tests in 2021–2025).
Surveillance should be intensified for groups at high risk of drug-resistant TB, including retreatment patients, those aged 25–44 years, patients with diabetes and TB, and Lengshuitan residents. A scale-up of molecular diagnostic technologies and increased testing panels to cover isoniazid resistance for accurate resistance assessment should be included. Post-pandemic TB control interventions should continue to optimize the quality of routine surveillance data, and in-depth research on non-laboratory factors that lead to regional disparities in drug resistance rates should be performed.
Dengue virus (DENV) and Zika virus (ZIKV), primarily transmitted by Aedes aegypti and Aedes albopictus, belong to the Flaviviridae family. Their clinical presentations overlap considerably, including acute fever, nausea, rash, joint pain, and myalgia, making differential diagnosis challenging.
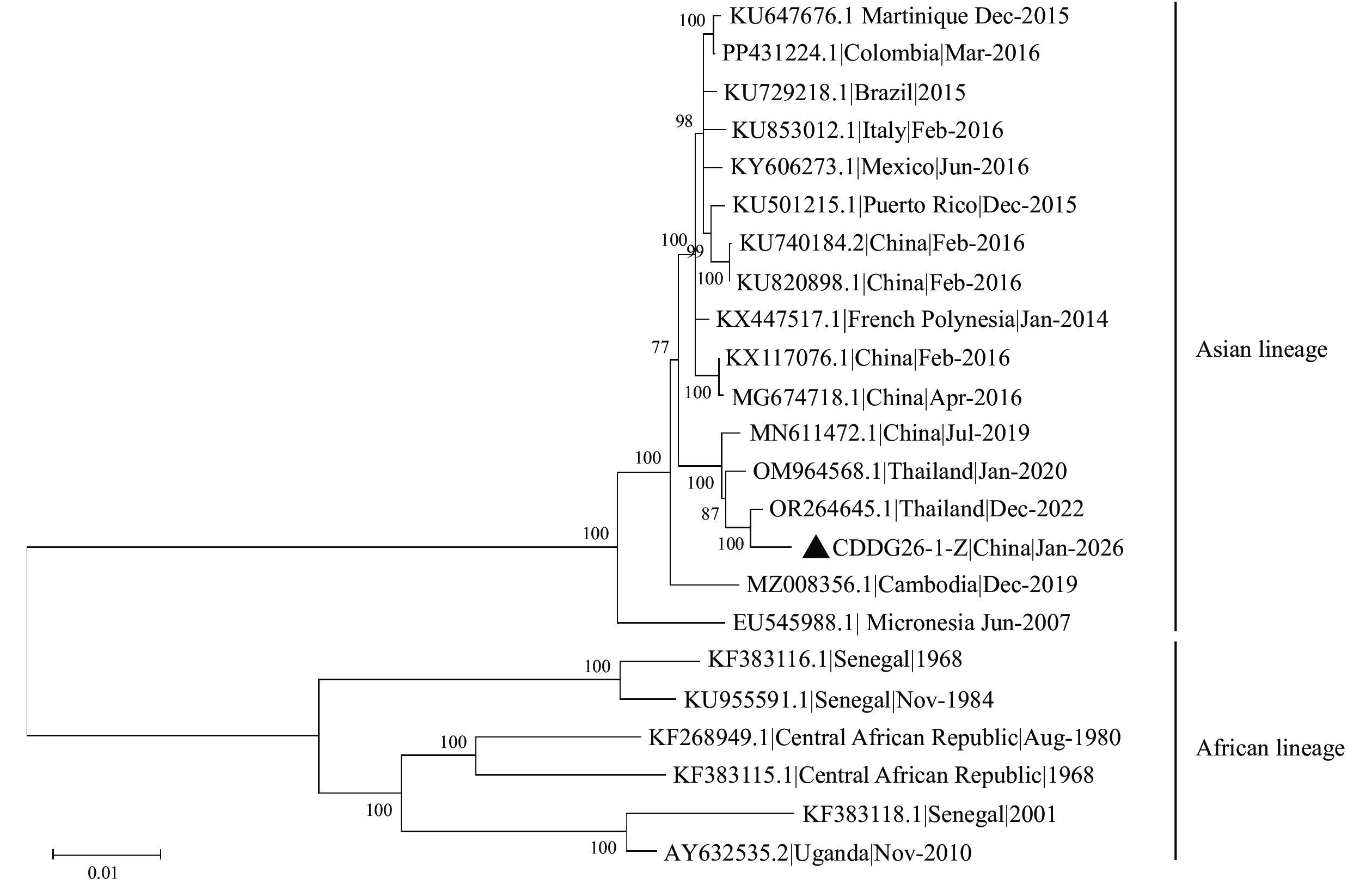
Because DENV and ZIKV share a common mosquito vector, their co-circulation increases the likelihood of dengue–Zika coinfection in both human and mosquito populations. This study documents the first laboratory-confirmed case of dengue/Zika coinfection in China. The patient presented with a fever on the day of entry.
This study provides a comprehensive epidemiological and phylogenetic analysis of a dengue/Zika coinfection case imported from Malaysia. Climate change and frequent cross-border travel are heightening the risk of imported mosquito-borne infectious diseases in China. International port cities must therefore strengthen surveillance and diagnostic testing for imported mosquito-borne diseases. For suspected febrile cases, clinicians should consider arbovirus coinfection based on travel history to prevent serious public health risks arising from missed diagnoses.



 Subscribe for E-mail Alerts
Subscribe for E-mail Alerts CCDC Weekly RSS Feed
CCDC Weekly RSS Feed