-
This perspective paper synthesizes current scientific evidence to argue that sleep health is not merely a matter of individual wellness, but a foundational pillar of public health and a key driver of health equity. By shifting from a narrow emphasis on clinical sleep disorders to a holistic public health framework, sleep health can be more effectively integrated into population-level strategies, strengthening chronic disease prevention and management.
-
The biological need for sleep is rooted in the circadian system, a highly conserved evolutionary mechanism that synchronizes internal physiology with the 24-hour light-dark cycle. Research underscores that the circadian clock acts as a central regulator of cardiac function and metabolic homeostasis. This internal timing system governs rhythmic fluctuations in blood pressure, heart rate, vascular tone, and hormone secretion. When these rhythms are disrupted, whether through shift work, sleep deprivation, or irregular behaviors, cellular oscillators become misaligned, triggering pathogenic pathways that lead to cardiovascular disease (CVD) (1).
The impact of sleep on the cardiovascular system is mediated through three primary systems: the autonomic nervous system, the metabolic system, and the immune system. Insufficient or disrupted sleep leads to sympathetic overactivity and the activation of inflammatory cascades.
Chronic sleep deficiency promotes the recruitment of inflammatory cells to the arterial walls, accelerating the development of atherosclerosis (2). Furthermore, sleep plays a pivotal role in “cardiovascular resilience”, allowing the heart and blood vessels to recover from daily physiological stressors. Consequently, sleep health must be prioritized as a biological imperative in public health strategies, equivalent to traditional metrics like nutrition and physical activity.
-
Historically, the medical community has viewed sleep through a “deficit-based” lens, focusing primarily on the diagnosis and treatment of specific disorders such as obstructive sleep apnea or insomnia. While identifying pathology is vital, this clinical approach often fails to address the sleep needs of the broader population. A paradigm shift toward “Sleep Health” provides a positive, holistic frame of reference (3). Sleep health is defined as a multidimensional pattern of sleep-wakefulness, adapted to individual, social, and environmental demands, that promotes physical and mental well-being (3-4).
The most widely accepted model for measuring sleep health is the RU-SATED framework (3,5), which evaluates six key dimensions:
Regularity: Consistency of bedtimes and wake times.
Satisfaction: Subjective sleep quality.
Alertness: Ability to sustain wakefulness during the day.
Timing: Alignment of sleep within the 24-hour cycle.
Efficiency: Ratio of time asleep to total time in bed.
Duration: Total sleep obtained within a 24-hour period.
Crucially, sleep health does not exist in isolation. A “translational neuroscience” perspective reveals that sleep is deeply embedded within its social and environmental context (4). Individual behaviors are shaped by societal structures — from labor laws and neighborhood safety to urban design. Adopting a contextual framework enables public health professionals to identify “upstream” determinants, such as light pollution and economic instability, that undermine optimal sleep.
-
Rapid societal transformation and urbanization have significantly challenged healthy sleep patterns. In the Chinese general population, sleep disturbances remain highly prevalent: a meta-analysis of 376,824 individuals reported a pooled prevalence of poor sleep quality of 19% (6), and the prevalence of insomnia symptoms and obstructive sleep apnea continue to rise (7). Reflecting sleep’s importance as a fundamental determinant of population health, several international consensus statements have elevated its priority. In 2022, the American Heart Association (AHA) updated its cardiovascular health construct from “Life’s Simple 7” to “Life’s Essential 8” by adding sleep duration as a key metric (8). This inclusion signals that sleep is now recognized as equally influential in CVD risk as blood pressure or lipid levels. A subsequent AHA scientific statement further delineated multidimensional sleep health — encompassing sleep duration, continuity, timing, regularity, sleep-related daytime functioning, architecture, and the absence of sleep disorders — and its relevance to cardiometabolic health (9). The AHA has also highlighted links between disturbed sleep and adverse neurological outcomes, including stroke, subclinical cerebrovascular disease, and Alzheimer’s disease (10), and has emphasized circadian health as a critical component of metabolic well-being (11).
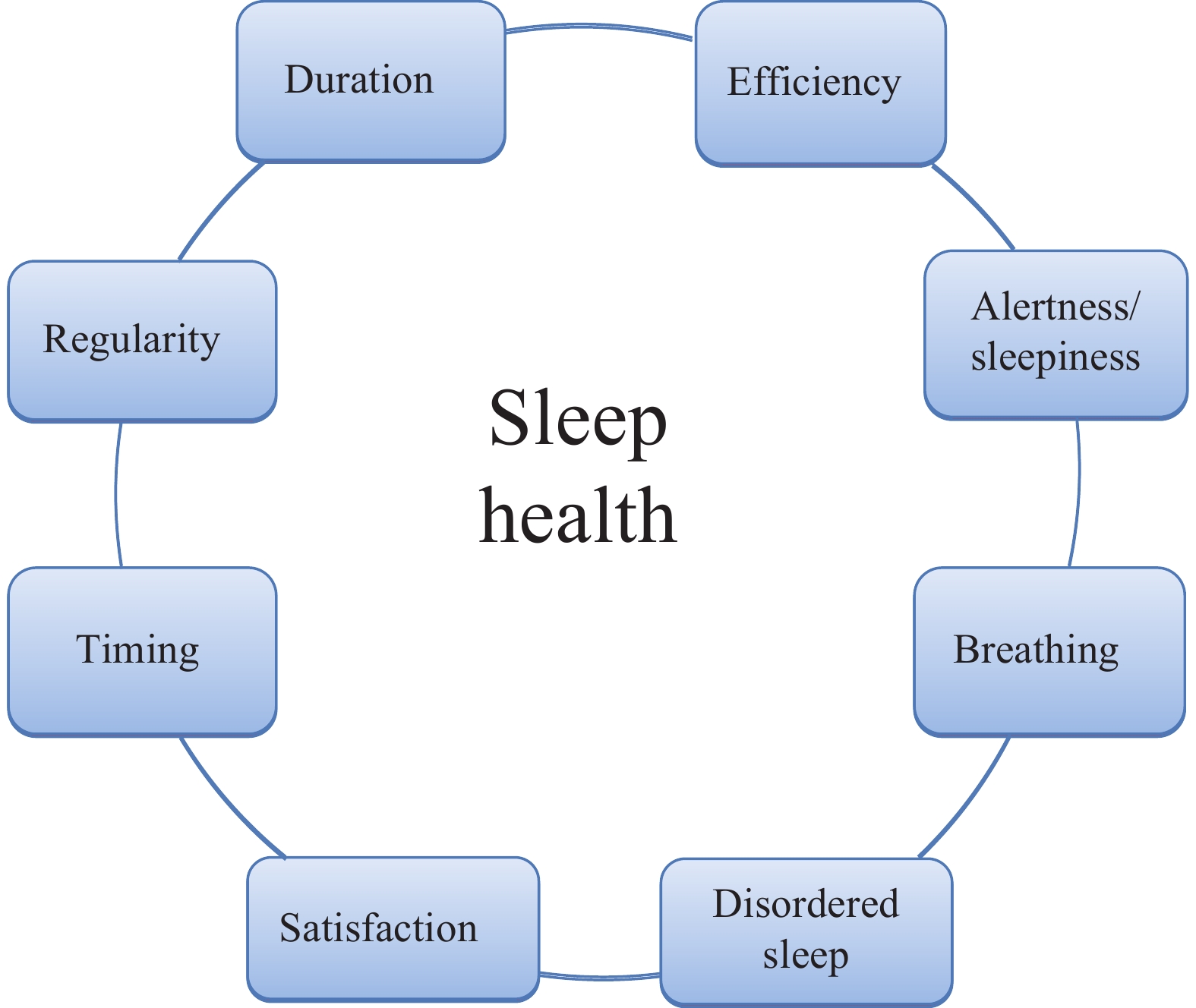
The World Sleep Society Global Sleep Health Taskforce has similarly called for integrating sleep into national public health agendas (12), arguing that the current neglect of sleep health — particularly in developing countries — constitutes a critical gap in global health policy. In Europe, an eight-component sleep health model incorporating additional domains related to breathing and disordered sleep has been proposed (Figure 1) (13). Ongoing efforts aim to synthesize data on the relationships between multidimensional sleep health, mortality, cardiovascular outcomes, and the socioeconomic impact of untreated sleep conditions (14). The recently released European Commission “Safe Hearts Plan” marks another milestone, advocating for the integration of sleep assessment into preventive care and public health monitoring across regional health systems.
A growing body of longitudinal evidence supports the transition to a multidimensional sleep health framework. Studies demonstrate that “healthy sleep scores,” which aggregate multiple sleep dimensions, outperform single metrics such as sleep duration in predicting cardiovascular risk (15). Tracking changes in these composite scores over time enables clinicians and public health officials to monitor shifts in population risk profiles. Notably, individuals who maintain or improve their sleep health scores exhibit significantly lower incidence of coronary heart disease and stroke.
Beyond physical health, sleep health is a major determinant of economic and functional outcomes. Recent studies have examined the relationship between multidimensional sleep health and work productivity, particularly among individuals with chronic conditions (16). In populations living with neurological disorders, poor sleep health — characterized by high fragmentation and low satisfaction — emerges as a significant predictor of reduced work performance and increased absenteeism. These findings suggest that promoting sleep health represents not only a medical imperative but also a strategy for enhancing societal productivity and reducing the economic burden of chronic illness.
-
It is evident that sleep health policies have begun to emerge in China. For example, sleep promotion has been incorporated into the Healthy China Action (2019–2030), which recommends an average daily sleep duration of 7–8 hours for adults and minimum sleep durations of 10, 9, and 8 hours for primary, junior high, and senior high school students, respectively. Nevertheless, additional efforts are required to further strengthen multidimensional sleep health promotion and advance health equity in China.
Currently, the “sleep gap” mirrors broader social inequalities: individuals from socially and economically marginalized backgrounds are disproportionately exposed to environmental stressors that degrade sleep quality (17). A socio-ecological framework is essential for addressing these disparities. This model recognizes that individual sleep is influenced by nested layers of influence: the social environment (e.g., family, work), the physical environment (e.g., noise, light), and the societal environment (e.g., policies). Looking forward, the research community has established a “roadmap” for the next decade of sleep health (18).
This roadmap prioritizes:
-
Understanding how sleep and circadian rhythms build “cardiovascular resilience” to protect against chronic stress.
-
Advocating for structural changes, such as the regulation of blue light in public spaces and the implementation of “circadian-friendly” work schedules.
-
Moving beyond individual-level sleep hygiene to implement structural and societal interventions that mitigate excessive work and social pressures and promote environments that support sufficient and high-quality sleep.
By treating sleep as a collective public health priority rather than an individual responsibility, we can close the sleep gap and improve health outcomes for the most vulnerable populations. Sleep is the new frontier for health equity, and its integration into the global public health agenda is no longer optional; it is essential for the future of human health.
HTML
Biological Foundation of Sleep and Circadian Health
From Sleep Disorders to Sleep Health
Global Consensus and Clinical Evidence
Future Perspectives
Mechanistic research:
Environmental policy:
Holistic approach:
| Citation: |



 Download:
Download:




