-
In Europe, population ageing poses a challenge. Given accelerating population ageing in Europe, long-term care (LTC) is a growing concern. Unmet healthcare needs varied among European countries during the coronavirus disease 2019 (COVID-19) pandemic, and greater attention should be paid to ensuring that the healthcare needs of vulnerable populations are met. Notably, developing common and comparable indicators is useful for monitoring the LTC and healthcare of older adults at the national and international levels, and understanding the reasons for the differences in indicators between European countries could shed light on how to improve the health of older adults. As such, in engaging with this challenge, this study uses a compilation of statistics that presents together, for the first time, three types of indicators relating to socioeconomic characteristics for population ageing, long-term care, and access to healthcare during the COVID-19 pandemic among the older adults in Europe (particularly in Belgium, Germany, Spain, France, Italy, and the Netherlands).
-
Indicators of socioeconomic characteristics for population ageing included older adults (65 years and over) as the percentage of total population, old-age dependency ratio and economic old-age dependency ratio (Table 1). In 2019, older adults aged 65 years and over comprised 20.4% of the total population in EU-27 countries, and this is predicted to increase to 29.6% by 2050. The old-age dependency ratio in EU-27 countries was 34.4% in 2019 and is estimated to rise to 56.9% by 2050. The economic old-age dependency ratio was 44.7% in 2019: which will likely increase to 69.5% by 2050. Among the 6 selected Western European countries, Italy has the highest share of older adults aged 65 years and over relative to the total population, as well as the highest old-age dependency ratio and economic old-age dependency ratio (1).
Indicator/year 2019 2030 2040 2050 2060 2070 Older adults (65 years and over) as the percentage of total population EU-27 20.4 24.4 27.7 29.6 30.3 30.3 BE 19.0 22.8 25.2 26.4 27.4 28.0 DE 21.7 25.6 27.9 28.1 28.3 28.4 ES 19.5 24.0 29.4 32.7 32.5 32.0 FR 20.3 24.1 26.8 27.8 28.3 28.7 IT 23.0 27.3 32.2 33.7 33.4 33.3 NL 19.3 23.7 26.3 26.4 27.3 28.6 Old-age dependency ratio EU-27 34.4 43.1 51.4 56.9 59.2 59.2 BE 32.5 40.5 46.0 49.2 51.8 53.3 DE 36.1 46.4 52.2 52.8 54.3 54.6 ES 32.1 40.9 54.0 64.7 64.1 62.5 FR 32.1 40.9 54.0 64.7 64.1 62.5 IT 38.9 48.0 61.4 66.5 65.5 65.6 NL 32.9 42.4 49.3 49.3 51.4 55.2 Economic old-age dependency ratio EU-27 44.7 53.9 63.3 69.5 71.9 71.7 BE 45.0 53.6 61.2 65.9 69.7 71.9 DE 41.9 52.4 59.8 60.7 62.1 62.7 ES 46.1 53.0 66.2 77.9 77.9 75.6 FR 46.1 53.0 66.2 77.9 77.9 75.6 IT 58.5 65.8 81.0 87.0 84.2 82.2 NL 37.6 48.2 56.5 56.0 57.0 60.5 Note: Old-age dependency ratio: population aged 65 years and over as a percentage of the population aged 20–64 years. Economic old-age dependency ratio: inactive population aged 65 years and over as a percentage of the employed population aged 20–64 years.
Abbreviation: BE=Belgium; DE=Germany; ES=Spain; FR=France; IT=Italy; NL=The Netherlands; EU-27=European Union with 27 Member States.Table 1. Main indicators of population ageing at average level in the EU and in selected countries in 2019–2070 (1).
Figure 1 shows the distribution of older adults aged 65 years and over according to their household type in selected European countries and in the EU for 2016–2020. At the average level across the EU-27 in 2019, the majority of such households consisted of either a single older adult (32.9%) or a couple living alone (47.9%), with a couple living with other people representing only 10% of over-65 households on average. In 2020, Germany had the highest percentage of households consisting of a single older adult (34.7%), the Netherlands had the highest percentage of households consisting of a couple living alone (63.7%), and Spain had the highest percentage of households consisting of a couple living with another person (18.6%) (2).
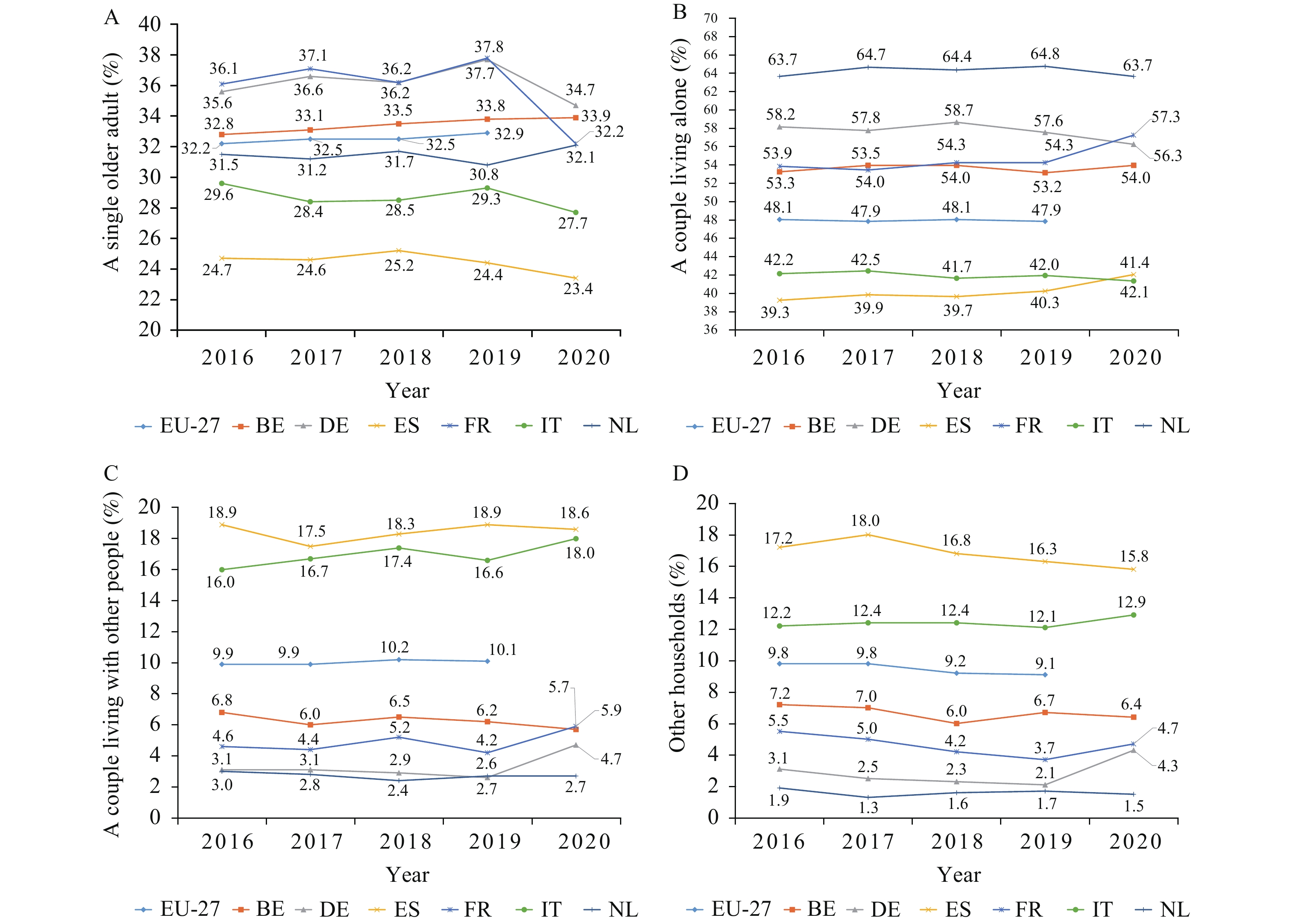 Figure 1.
Figure 1.Distribution of older adults aged 65 years and over according to household type in selected European countries and in the EU from 2016–2020. (A) Percentage of household type in a single older adult by year; (B) Percentage of household type in a couple living alone by year; (C) Percentage of household type in a couple living with other people by year; (D) Percentage of household type in other households by year (2).
Abbreviation: BE=Belgium; DE=Germany; ES=Spain; FR=France; IT=Italy; NL=The Netherlands; EU-27=European Union with 27 Member States.The average retirement age for women and men across the EU-27 was approximately 65 years. As of 2022, the average retirement age was 62 years in France; 65 years in Belgium; 65 years and 3 months in Spain; 65 years and 7 months in Germany; 66 years and 4 months in the Netherlands; and 67 years in Italy. Additionally, the retirement age in Belgium, Spain, and Germany will rise to 67 years in 2030, 2027, and 2029 respectively (3).
-
LTC encompasses a variety of services designed to meet the health and personal care needs of older adults, with the goal of enabling them to live as independently and safely as possible (4). Indicators related to LTC are categorized in terms of need, access, workforce, and expenditure, according to the European Commission Social Protection Committee, and are summarized in Table 2 (5). In 2014, 27.3% of older adults aged 65 years and over needed LTC in the EU-27. In 2019, 9.4% of older adults received LTC, with 3.6% receiving care in LTC facilities, 5.8% receiving care at home, and 8.8% receiving LTC cash benefits. Of the 45.4% who needed home care services but did not receive them, for 35.7% this was due to financial reasons, while for 9.7% it was because the services were unavailable. The number of employees in LTC was 3.8 per 100 older adults aged 65 years and over in the EU-27 in 2016, while 10.3% of the population provided informal care for older adults. EU-27 public expenditure on LTC was 1.7% of gross domestic product (GDP) in 2019 and is projected to reach 3.4% of GDP by 2050.
Item EU-27 BE DE ES FR IT NL Need of long-term care A1 27.3* 29.9 15.2* 28.8 21.5 28.7 26.9 Access to long-term care B1 3.6 6.2 4.3 1.2 4.9 3.2 5.6 B2 5.8 15.7 3.6 3.9 6.2 4.7 19.1 B3 8.8 7.8 11.3 4.4 0 10.9 1.2 B4 51.8* NA 72.1* 47.9 38.7 44.2 24.5 B5 11.0* 25.1 6.3* 10.8 15.1 9.5 18.0 B6 35.7† 24.4 19.2† 54.1 16.4 36.9 30.3† B7 9.7† 5.8 3.8† 7.3 3.6 30.3 8.3† B8 NA 1276.6 1152.2 830.3 981.5 415.8 1370.7 Long-term care workforce C1 3.8† 4.8† 5.1† 4.5† 2.3† 1.9† 8.0† C2 10.3† 11.6† 6.8† 11.5† 14.1† 5.8† 36.7† C3 22.2† 15.0† 15.0† 52.9† 10.5† 40.5† 3.3† Public long-term care expenditure as the percentage of GDP D1 1.7 2.2 1.6 0.7 1.9 1.7 3.7 D2 2.1 2.7 1.9 1.0 2.3 2.0 4.7 D3 3.4 4.4 2.8 2.1 3.7 3.1 6.7 D4 48.1 62.5 35.7 50.2 69.6 28.2 51.0 D5 25.5 26.8 23.5 25.9 24.8 19.5 16.4 D6 26.4 10.7 40.8 23.9 5.6 52.3 32.6 Note: A1 = The percentage of population aged 65 years and over requiring long-term care.
B1 = The percentage of population aged 65 years and over receiving care in long-term care facilities.
B2 = The percentage of population aged 65 years and over receiving care at home.
B3 = The percentage of population aged 65 years and over receiving long-term care cash benefits.
B4 = The percentage of population aged 65 years and over in need of long-term care with a lack of assistance in personal care or household tasks.
B5 = The percentage of population aged 65 years and over who have used home care services for personal needs in the past 12 months.
B6 = The percentage of population aged 65 years and over in need of long-term care, but not using (more) professional home care services due to the financial reason.
B7 = The percentage of population aged 65 years and over in need of long-term care, but not using (more) professional home care services because the services needed are not available.
B8 = Beds for long-term care per 100,000 residents.
C1 = Number of long-term care (formal care) workforce per 100 older adults aged 65 years and over.
C2 = The percentage of population providing informal care, which is the proportion of respondents who provide care or assistance to one or more individuals requiring assistance due to long-term physical or mental illness, physical weakness, or old age. Only unpaid, volunteer assistance is considered.
C3 = The percentage of informal carers providing more than 20 hours informal care per week.
D1 = Public long-term care expenditure as % of gross domestic product (GDP) in 2019.
D2 = Public long-term care expenditure as % of GDP projected for 2030.
D3 = Public long-term care expenditure as % of GDP projected for 2050.
D4 = Public expenditure on institutional care as % of total public long-term care expenditure.
D5 = Public expenditure on home care as % of total public long-term care expenditure.
D6 = Public expenditure on cash benefits as % of total public long-term care expenditure.
Abbreviation: BE=Belgium; DE=Germany; ES=Spain; FR=France; IT=Italy; NL=The Netherlands; EU-27=European Union with 27 Member States; NA indicates that data were unavailable.
* Indicates that the data came from 2014.
† Indicates that the data came from 2016.
Table 2. Need, access, workforce, and expenditure of long-term care for older adults for the EU population and selected European countries in 2019 (5).
There are some differences between countries. For instance, the proportion of older adults in Belgium aged 65 years and over requiring LTC (29.9%) was higher than in other selected European nations. In addition, in 2019 a greater proportion of older adults in Belgium received LTC in LTC facilities (6.2%) or at home (15.7%) than in other countries. In 2019, the number of LTC beds per 100,000 residents in both the Netherlands and Belgium exceeded 1,200, which was significantly higher than in other nations. In comparison to other nations, the Netherlands had 8 LTC employees for every 100 older adults aged 65 years and over. Moreover, in 2019, the Netherlands had the highest public expenditure on LTC, accounting for 3.7% of GDP.
-
Unmet healthcare needs are defined as the difference between the quantity of care received and the quantity of care desired or required, which typically take three forms: giving up, postponement, and inaccessibility (6). The indicators for unmet healthcare needs during the COVID-19 pandemic included refusing healthcare out of fear of COVID-19, postponing planned healthcare, and inability to obtain medical treatment or appointment, as developed by the Survey of Health, Ageing and Retirement in Europe (SHARE) Corona Survey (7). Figure 2 shows the unmet healthcare needs during the first wave of the pandemic among adults aged 50 years and over. The majority of unmet healthcare needs in Europe resulted from postponing planned care, which accounted for 25%, followed by refusal of medical care due to fear of COVID-19 (12%) and inability to obtain medical treatment or an appointment (5%). There were differences across the selected countries. In France and Belgium, 36% and 35% of those aged 50 years and over postponed planned healthcare, respectively. In both Germany and Italy, 17% of those aged 50 years and over refused healthcare out of fear of COVID-19, which was higher than in other countries. In France and Belgium, 10% and 9% of those aged 50 years and over were unable to obtain medical treatment or an appointment, respectively. Additionally, frail populations were more likely to have unmet healthcare needs. For example, individuals aged 85 years and over were more likely to have unmet healthcare needs. Women were more likely to forgo healthcare for fear of COVID-19 and to postpone planned care. Populations who were economically vulnerable and self-rated as having poor health were also more likely to forgo healthcare for fear of COVID-19 and to postpone planned care (7).
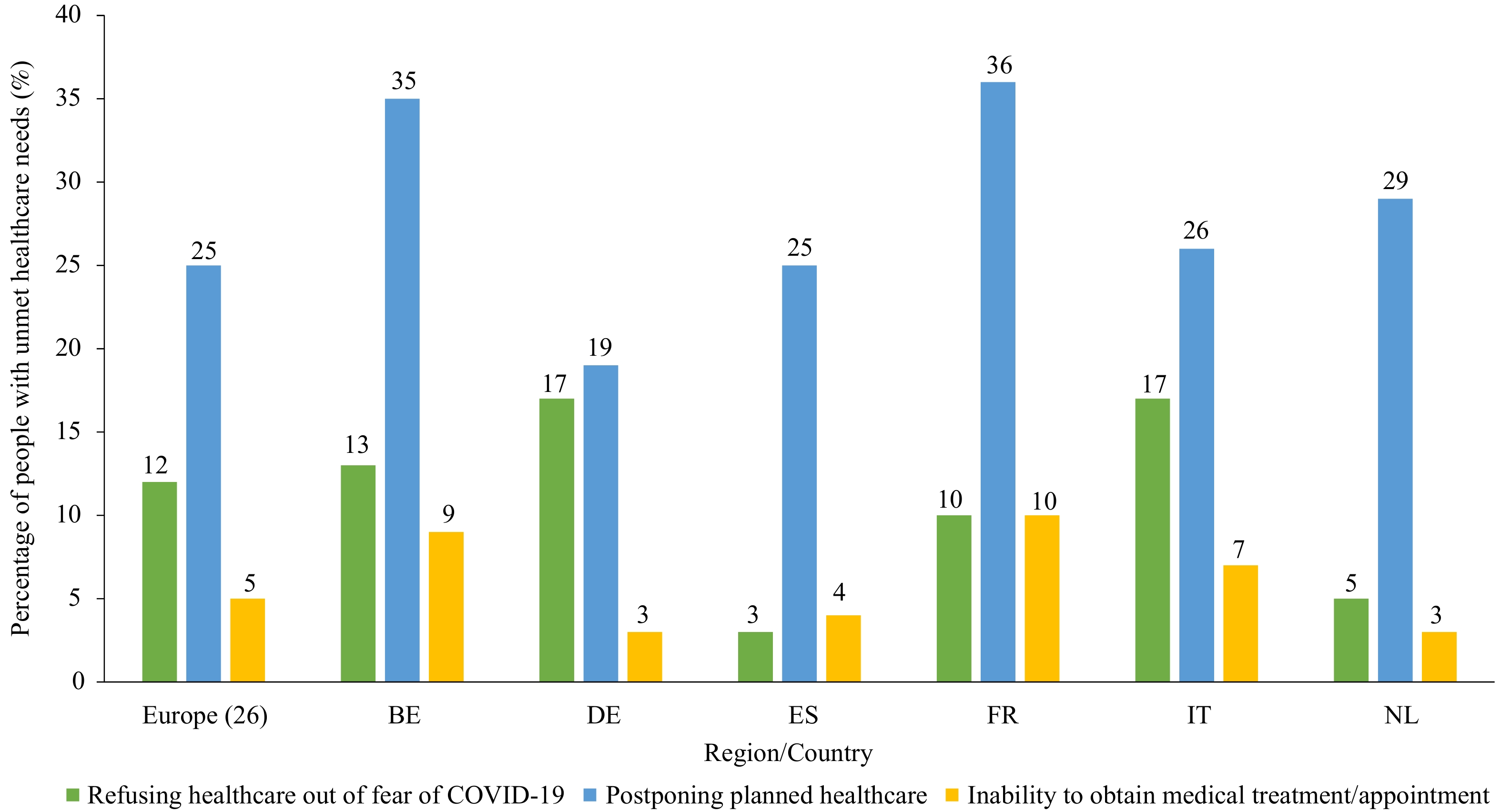 Figure 2.
Figure 2.Unmet healthcare needs during the first wave of the pandemic among adults aged 50 years and over in Europe and selected European countries. (7)
Note: Europe including Member States: Germany, Sweden, The Netherlands, Spain, Italy, France, Denmark, Greece, Switzerland, Belgium, Israel, Czech Republic, Poland, Luxemburg, Hungary, Slovenia, Estonia, Croatia, Lithuania, Bulgaria, Cyprus, Finland, Latvia, Malta, Romania and Slovakia.
Abbreviation: BE=Belgium; DE=Germany; ES=Spain; FR=France; IT=Italy; NL=The Netherlands.
-
To the best of our knowledge, this is the first time that these three types of indicators, including population ageing, long-term care, and unmet healthcare needs during the COVID-19 pandemic, have been examined together. Developing common and comparable indicators is useful for monitoring the healthcare of older adults at the national and international level. For example, Europe has summarized an evaluation index system for healthcare and LTC, which can be used for international comparisons, as well as by developing nations to allocate medical resources for older adults and monitor and enhance their care. As another example, LTC expenditures as a percentage of GDP, the ratio for LTC employees, and LTC beds in Europe were all much higher than in developing nations (5,8), and developing nations could use these indicators as a benchmark for allocating and enhancing healthcare and LTC for older adults. In addition, understanding the reasons for the differences in indicators between European countries can provide insight into ways to improve older adults’ health.
Developing indicators to monitor and improve care for older adults is a global challenge. Several indicators have been developed, but they do not fully meet the requirements for monitoring and enhancing care in Europe (9). In addition, the World Health Organization recommends that a global agreement on a standard set of care indicators be reached (10). Future development of a set of international and comparable indicators will be a crucial step in enhancing the quality of care for older adults worldwide, and this study helps contribute towards laying the groundwork for such a setup.
HTML
| Citation: |



 Download:
Download:




