-
The antimicrobial resistance characteristics of Vibrio parahaemolyticus (V. parahaemolyticus)
was studied by isolating the bacterium from diarrheal patients in 6 provincial-level administrative divisions (PLADs) from 2016 to 2020 reported to National Foodborne Disease Molecular Tracing Network (TraNet). A total of 2,871 clinical V. parahaemolyticus isolates were examined in this study, and the levels of resistance and multidrug resistance were compared within several epidemiological dimensions. The results demonstrated that V. parahaemolyticus isolates had high levels of resistance to cefazolin and ampicillin, and the other 10 tested antimicrobial agents including imipenem had similar levels of resistance, which were all below 3%. The distribution of antimicrobial resistance and/or the multidrug-resistance level had regional and temporal characteristics, with significant differences in sex and isolated source strain dimensions. These results demonstrated that V. parahaemolyticus isolates had high levels of drug resistance to some drugs and emerging resistance to many more, including carbapenem, and thus constitute a serious health risk. This study added to the knowledge of resistance in clinical V. parahaemolyticus isolates in China, which would help provide scientific epidemiological data, guide healthcare treatment of the disease, and develop a public health strategy accordingly. V. parahaemolyticus can cause sporadic infection in milder forms of gastroenteritis or large-scale food-related outbreaks (1-3). Antimicrobial resistance as well as other information of V. parahaemolyticus is required to be submitted to TraNet for analysis based on the existing laboratory-based foodborne disease surveillance system in China. V. parahaemolyticus were isolated by network laboratories from stool samples or rectal swabs collected from diarrheal patients who were either linked to outbreaks or were sporadic cases, seek medical care in hospitals in Beijing, Guangdong, Jiangsu, Shanxi, Tianjin, and Zhejiang from 2016 to 2020. To ensure the quality and comparability of the submitted surveillance data, they were processed in local laboratories following procedures to isolate V. parahaemolyticus strains and perform antimicrobial susceptibility testing in accordance with the standard operation procedures regulated by the national laboratory manual for foodborne disease surveillance system and TraNet. The analysis also included temporal and regional patterns, serotype distribution, and the correlation of susceptibility status with epidemiological dimensions that may contribute to develop a public health strategy. A panel of 12 antimicrobials belonging to 9 classes were selected for resistance analysis: gentamicin, cefazolin, cefotaxime, ceftazidime, cefoxitin, ciprofloxacin, imipenem, ampicillin, ampicillin/sulbactam, chloramphenicol, trimethoprim-sulfamethoxazole, and tetracycline. Isolates that were resistant to at least 1 of these 12 agents were considered resistant (R), and multiple drug resistance (MDR) was defined as “acquired resistance to three or more classes of antimicrobials.” Descriptive statistics were used to analyze the resistance prevalence to different antimicrobial agents. Pearson chi-square, continuous correction chi-square, or the likelihood ratio test were applied to test whether observed resistance level differences were statistically significant (P-values ≤0.05).
The temporal and spatial distribution of the strains isolated were shown in Figure 1. The incidence of V. parahaemolyticus isolated from diarrheal patients peaked in the warmer months from May to September in each of the six PLADs. Of the total 2,871 isolates, 95.1% (2,731/2,871) were resistant to at least 1 agent among the 12 tested antimicrobials; 3.3% of strains (94/2,871) were resistant to more than 3, and up to 8 classes, of antimicrobials, demonstrating a variety of 47 resistance patterns, and were defined as MDR strains in this study accordingly. A significant difference among different years was observed in the resistance percentage (R%), with 2017 showing the lowest percent (91.1%) and 2016 showing the highest (99.0%). Although differences by year were not significant, 2017 showed the highest MDR level (4.8%). Although also not significant, the R% and MDR percentage (MDR%) of V. parahaemolyticus by month showed that the drug resistance percentages isolated in July were relatively lower than those in the other months, especially in 2016 and 2020, and that higher percentages of MDR% were observed in July and August.
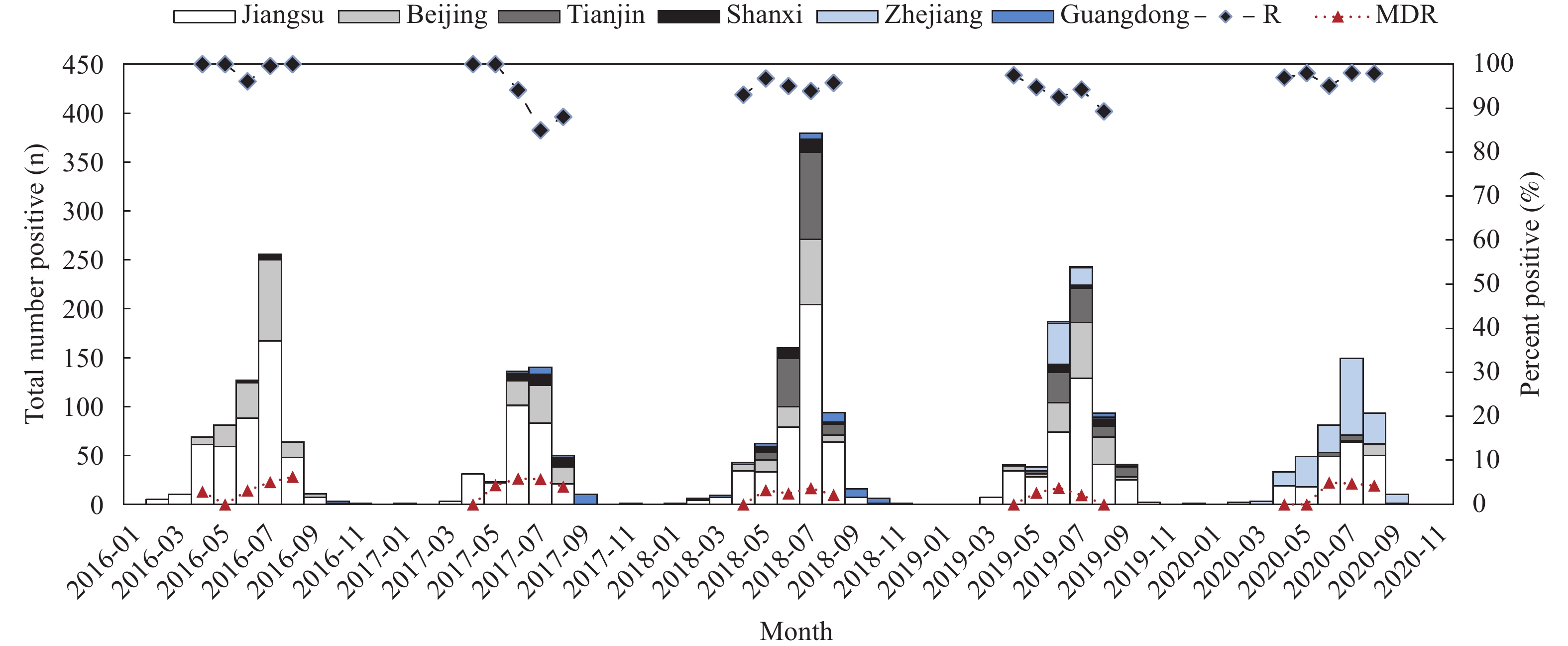 Figure 1.
Figure 1.The temporal and spatial distribution of V. parahaemolyticus positive tests, and R% and MDR% in 6 PLADs, China, 2016–2020.
R% is the percent of isolates that were resistant to at least one of 12 agents, and MDR% is the percent of resistance to 3 or more classes of antimicrobials.The levels of resistance to the 12 antimicrobials of the 2,871 examined V. parahaemolyticus isolated from diarrheal patients differed by region, as shown in Table 1. The majority of isolates tested were resistant to cefazolin, found in 94.4% (2,711/2,871) of the strains. Isolates were also commonly resistant to ampicillin (37.0%). Only few strains were resistant to the clinically relevant agents of cefotaxime, ceftazidime, and tetracycline (1.3%, 0.8%, and 2.6%). There is an emerging resistance to imipenem showed by 16 strains resistant and 8 strains intermediate. Low resistance levels (from 0.6% to 1.9%) were found to the 6 remaining antimicrobials: ampicillin/sulbactam, ciprofloxacin, gentamicin, cefoxitin, chloramphenicol, and trimethoprim-sulfamethoxazole. In addition, 94.6% (2,717/2,871) of strains exhibited resistance to at least one of the drugs classified as highly important antimicrobials, while 38.3% (1,100/2,871) of strains exhibited resistance to drugs classified as critically important antimicrobials by the World Health Organization (WHO). There was a significant difference in resistance to the drug agents ampicillin, cefotaxime, ceftazidime, cefazolin, cefoxitin, tetracycline, and trimethoprim-sulfamethoxazole by different PLADs.
Antimicrobial classes categorized by WHO* Antimicrobials MIC interpretive standard of resistance (µg/mL) R%† differed by PLADs P Overall R%† Beijing Guangdong Jiangsu Shanxi Tianjin Zhejiang Critically important antimicrobials Ampicillin (AMP) ≥32 22.5 54.6 50.9 11.5 8.9 7.6 <0.05 37.0 Ampicillin/sulbactam (AMS) ≥32/16 2.2 0.0 0.9 0.0 0.8 0.4 1.0 Cefotaxime (CTX) ≥4 2.4 0.0 0.7 5.8 1.9 0.8 <0.05 1.3 Ceftazidime (CAZ) ≥16 2.2 0.0 0.5 0.0 0.4 1.1 <0.05 0.8 Ciprofloxacin (CIP) ≥4 1.0 0.0 1.2 2.3 0.8 0.0 1.0 Gentamicin (GEN) ≥16 1.0 0.0 0.5 2.3 0.0 0.0 0.6 Imipenem (IPM) ≥4 1.2 0.0 0.8 0.0 0.4 0.4 0.7 Highly important antimicrobials Cefazolin (CFZ) ≥4 88.3 96.1 96.6 93.1 89.2 97.7 <0.05 94.4 Cefoxitin (CFX) ≥32 0.8 0.0 0.7 0.0 3.1 1.1 <0.05 0.9 Chloramphenicol (CHL)§ ≥32 2.4 0.0 1.1 1.2 0.8 0.4 1.2 Tetracycline (TET) ≥16 4.0 0.0 2.0 6.9 4.3 1.5 <0.05 2.6 Trimethoprim-sulfamethoxazole (TMP-SMX) ≥4/76 2.6 0.0 1.7 5.8 2.7 0.8 <0.05 1.9 Abbreviations: PLADs=provincial-level administrative divisions; MIC=minimum inhibitory concentration.
* Seven antimicrobials were classified by the WHO as critically important antimicrobials and five as highly-important antimicrobials.
† R% means the percent of isolates that were resistant to at least one of 12 agents.
§ No CLSI break point for V. parahaemolyticus applied MIC ≥32 μg/mL as for Vibrio cholerae.Table 1. Resistance of V. parahaemolyticus isolates to 12 antimicrobials tested differed by region.
Table 2 shows the distribution of characteristics of antimicrobial resistance levels of V. parahaemolyticus in terms of epidemiological dimensions. A significant difference in R% and MDR% of V. parahaemolyticus by sample locations was observed. The highest R% were observed in Zhejiang and the lowest in Beijing. The highest level of MDR was observed in Shanxi, and in Guangdong no MDR was found. It seemed that the northern PLADs (Beijing, Tianjin, and Shanxi) had relative lower R% and higher MDR%, and the southern PLADs (Guangdong, Jiangsu, and Zhejiang) had higher R% and lower MDR%. There were significant differences in MDR between male and female patients, with strains originating from females exhibiting higher levels, while no significant differences in drug resistance. Strains isolated from outbreak related-cases and from sporadic patients had significant differences in both the drug and multidrug-resistant level, with outbreak related-isolates having higher R% and lower MDR%. Although there was no significant difference, V. parahaemolyticus identified as O4:K8 serotypes had higher D% and MDR% compared with serotype O3:K6 strains.
Variable No. of tested strains R% P MDR% P PLADs <0.05 <0.05 Beijing 503 89.3 4.8 Guangdong 77 96.1 0.0 Jiangsu 1,680 97.2 3.2 Shanxi 87 94.3 5.8 Tianjin 259 90.4 3.1 Zhejiang 265 97.7 1.1 Gender* >0.05 <0.05 Men 1,127 95.4 3.1 Women 995 95.8 5.0 Strain source† <0.05 <0.05 Outbreak 362 99.2 0.8 Patient 2,086 95.0 3.7 Serotype§ >0.05 >0.05 O3:K6 421 91.2 2.6 O4:K8 59 94.9 5.1 Note: R% is the percent of isolates that were resistant to at least one of 12 agents, and MDR% is the percent of resistance to 3 or more classes of antimicrobials.
Abbreviation: PLADs=provincial-level administrative divisions.
* There were some missing values (749) for gender.
† In order to balance the difference between different regions, the strains included here were from the same PLADs.
§ Only a limited number of strains had available information on serotype and among which 480 isolates were identified as either O3:K6 or O4:K8.Table 2. Association between epidemiological dimensions, resistance, and multidrug-resistance in 2,871 V. parahaemolyticus strains from patients.
-
The results of this study showed that V. parahaemolyticus isolated from patients in 6 PLADs of China have a R% of 95.1%, and it also showed a 3.3% MDR% and multiple antimicrobial resistances of up to 8 classes of antimicrobials. Our findings placed cefazolin at the top of the clinical V. parahaemolyticus resistance (94.4%), which was much higher than previous results (4-5). Especially alarming was the emergence of imipenem intermediate and resistant V. parahaemolyticus strains, which had not previously been reported in China. Imipenem belongs to the carbapenem class and has always been regarded as the last treatment option for the treatment of bacterial infection (6). These results highlight the negative impact of carbapenem misuse, which may cause failure of the clinical treatment of Vibrio and other infections in the future.
Resistance was found in V. parahaemolyticus to all 12 antimicrobials tested, which was in contradiction to other studies on V. parahaemolyticus showing that it remained highly susceptible to many antimicrobial agents except for ampicillin and streptomycin (4-5, 7-9). Tetracycline, ciprofloxacin, cefotaxime, ceftazidime, gentamicin, and trimethoprim-sulfamethoxazole were the antimicrobial agents that were recommended for use in the treatment of Vibrio spp
. infections (10). Although the resistance level was relatively low, those six clinically-applied antimicrobials were considered as constituting the defense against V. parahaemolyticus infections, so even a small percentage of resistance isolates could be cause for concern. In this context, the current treatment guidelines should be re-assessed, and surveillance and monitoring of antimicrobial usage and resistance should be enhanced to make sure the drug is employed only with great caution. This study demonstrated a difference in the drug resistance levels and multiple drug resistance levels of V. parahaemolyticus according to several external factors. The drug resistance levels of V. parahaemolyticus seems related to the month of isolation, which may be related to the survival adaptability of V. parahaemolyticus strains with different resistant capabilities in different meteorological conditions. In terms of regional distribution, the highest drug resistance levels were found in Zhejiang and MDR in Shanxi. The MDR level of female patients was higher than that of male patients. These differences may result from different drug use habits and food habits especially towards aquatic products and other unknown factors.
This study was subject to at least some limitations. First, the top six PLADs that isolated the most V. parahaemolyticus were included in this study and were therefore not representative of the country. Second, antimicrobial susceptibility testing was processed in local laboratories and may bring some variation in the results.
In summary, the study showed that the clinical protocol to treat V. parahaemolyticus infection should be selected on the basis of a drug sensitivity testing since clinically relevant agents recommended were no longer completely effective. Both imipenem-resistant and multiple antimicrobial-resistant V. parahaemolyticus strains pose a great challenge to the treatment of the disease and public health problems caused by V. parahaemolyticus, which needs to be of wide concern to governmental departments and health institutions worldwide. The differences between external factors may give clues to the formulation of policies to prevent infection and to design related research to unveil the underlying mechanisms.
Conflicts of interest: No conflicts of interest.
Acknowledgements: All research staffs from local Centers for Disease Control and Prevention for participation and contribution. Jean Marie Whichard who worked at the Centers for Disease Control and Prevention in the Division of Foodborne, Waterborne, and Environmental Diseases for providing professional revision advisements.
HTML
| Citation: |



 Download:
Download:




