-
The influenza virus causes contagious acute respiratory disease with considerable morbidity and mortality in general population worldwide. The World Health Organization (WHO) estimates that 5%–10% of the world population each year becomes infected with the seasonal influenza virus, mainly influenza A and B viruses, resulting in approximately one billion influenza cases (1), 3–5 million cases of severe illness, and 290,000–650,000 fatal cases (2). So far, there have been four influenza pandemics in history caused by the influenza A virus including the 1918 Spanish flu [A(H1N1)], the 1957 Asian flu [A(H2N2)], the 1968 Hong Kong flu [A(H3N2)], and the 2009 swine-origin flu [A(H1N1) pdm09] (3). Meanwhile, influenza B has caused many local outbreaks with high morbidity and mortality (4), and in some epidemic seasons, the influenza B virus disease burden actually exceeds that of the influenza A virus.
Because influenza viruses are prone to immunogenic changes, the WHO annually recommends specific vaccine strains in preparation for the next epidemic. In addition to the influenza A viruses H1N1 and H3N2, two different genetic lineages of influenza B virus B/Victoria and B/Yamagata have been co-transmitted worldwide since the 1980s (5-6). At the end of the 2017–2018 influenza season, the Chinese National Influenza Center (CNIC) reported that the influenza B epidemic in China was mainly B/Yamagata lineage strains, so an inactivated, quadrivalent split-virion influenza vaccine (IIV4s) has been developed containing one A/H1N1 strain, one A/H3N2 strain, and two B strains from B/Victoria and B/Yamagata lineages. The first domestically produced quadrivalent split influenza vaccine was launched in China in June 2018. Both the trivalent and quadrivalent influenza vaccines were used in the following 2018–2019 season. The comparison of the immune effects of the two vaccines among the population needs further investigation (7). Important indicators of the vaccines, such as the post-vaccination seroconversion rate, protective antibody titer, and immunity duration, deserve timely surveillance.
Subjects were enrolled using random cluster sampling. In a community of Shenzhen, 75 subjects were vaccinated with domestically-produced quadrivalent split influenza vaccine, and 30 participants were recruited as controls (not vaccinated with any component). In a community of Changzhou, 74 volunteers were vaccinated the trivalent split influenza vaccine, and 38 participants were selected as controls (Figure 1A). The volunteers enrolled in the study were healthy with no contraindications to influenza vaccinations, and the children’s guardian gave informed consent. To reflect the natural effects of the vaccines, the vaccines used for the study subjects were local vaccines available in different cities. The information of the vaccines was available under request. The study was approved by the Ethics Review Committee of National Institute for Viral Disease Control and Prevention, China CDC. The study was conducted in accordance with the principles of the Declaration of Helsinki and the standards of good clinical practice as defined by the International Conference on Harmonization. After obtaining written informed consent, the subjects were interviewed and given questionnaires, then followed up regularly.
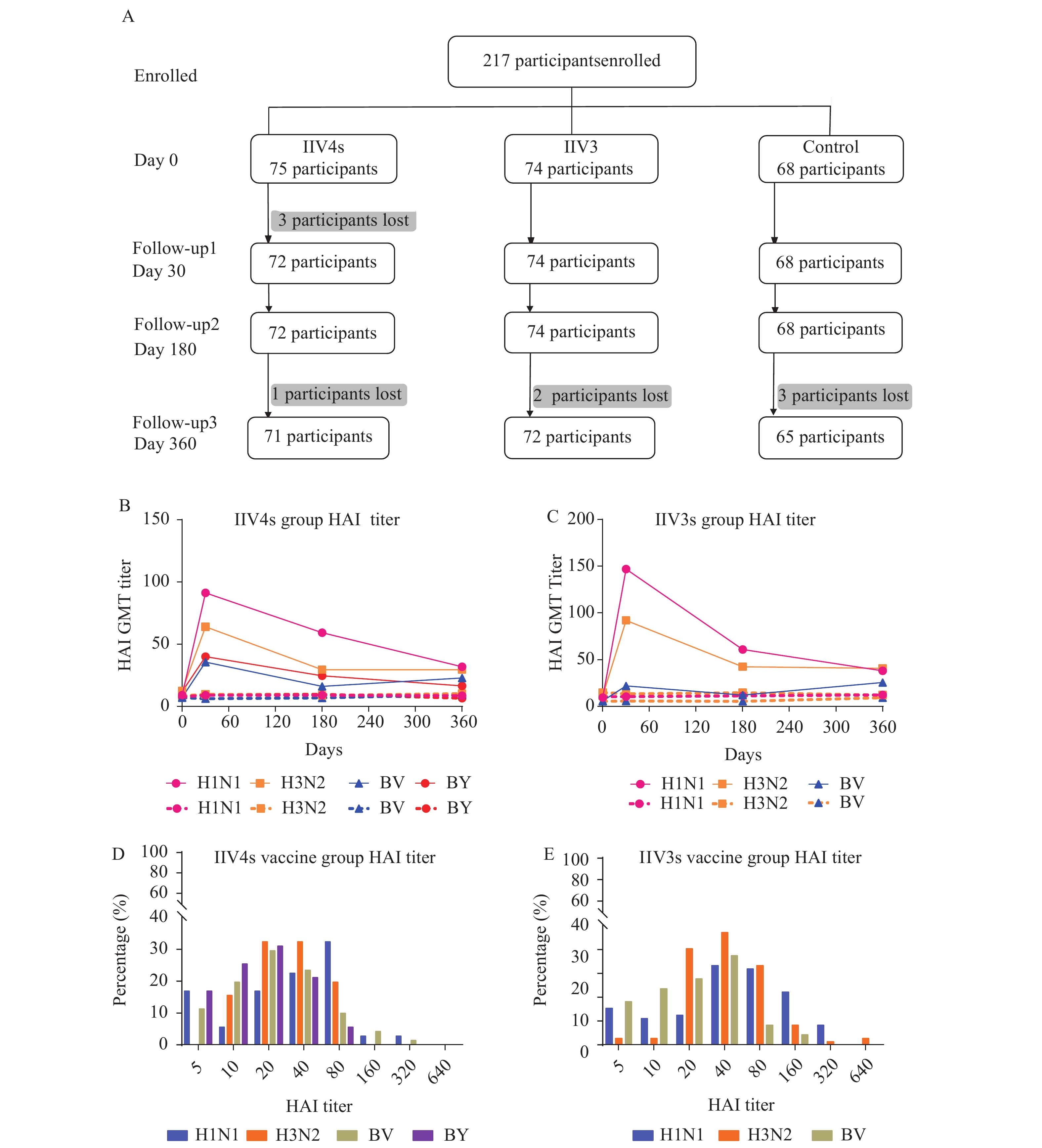 Figure 1.
Figure 1.Monitoring flow chart and antibody levels in the monitored subjects in Shenzhen and Changzhou, 2018–2019. (A) Flowchart of initial participant enrollment and follow-up distribution among different group in the study of surveillance on the immune effectiveness of quadrivalent and trivalent split influenza vaccines in southern China, 2018–2019 season. (B) Quadrivalent (IIV4s) vaccines group and control group antibody change trends. (The solid line represents the vaccine group and the dotted line represents the control group). (C) Trivalent (IIV3s) vaccines group and control group antibody change trends. (D) Quadrivalent (IIV4s) vaccines group serum antibody levels percentage in 360-day. (E) Trivalent (IIV3s) vaccines group serum antibody levels percentage in 360-day. HAI=hemagglutination inhibition; BV=B/Victoria; BY=B/Yamagata.
Venous blood was collected from subjects a total of four times: on Day 0 before vaccination, at Day 30, Day 180, and Day 360 post-vaccination. Sera were isolated from these samples, and serum preparation steps were performed with reference to the “National Influenza Surveillance Technology Guide (2017 Edition)” of CNIC as previously reported (8). The hemagglutination inhibition titer (HAI) was used to evaluate the immunogenicity of seasonal influenza vaccine components. Four agglutination unit antigens were prepared from chicken embryo-adapted strains: A/Michigan/45/2015 (H1N1), A/Singapore/INFIMH-16-0019/2016 (H3N2), B/Colorado/06/2017 (B/Victoria), and B/Phuket/3073/2013 (B/Yamagata). Positive control serum was prepared as described previously (9). The HAI titer was calculated as the reciprocal of the serum dilution at which erythrocyte agglutination is inhibited in turkey red blood cells. Seroconversion was defined in accordance with the European Medicines Agency (EMA) criteria (10): HAI titers of <10 at baseline and ≥40 at Day 30 post-vaccination, of >10 at baseline with at least a four-fold increase from baseline at Day 30 post-vaccination, or when HAI titer <1:10 then calculate geometric mean titer (GMT) according to 1:5.
A database of the subject and sample information was established using EpiData (version 3.1, EpiData Software, Epi Info V6, Denmark), and the questionnaire data were entered in parallel. Statistical analyses were performed using SAS® (version 9.4, SAS Institute, Cary, NC, USA). A one-way analysis using a chi-square test and a multi-factor analysis using non-conditional logistic regression were performed to analyze the factors affecting the seroconversion rates among subjects. Test level significance was set at α=0.05. Graphs were generated using GraphPad Prism (version 7.0, GraphPad Software Inc., San Diego, CA, USA) and Excel 2016 ( version 2016, Microsoft Corporation, Redmond, WA, USA).
Subject enrollment began on November 20, 2018, and a total of 217 subjects were monitored through December 8, 2019. A total of 75 subjects were inoculated with IIV4s with 36% (27/75) male and 64% (48/75) female. The basic information of the study subject was shown in the Supplementary Table S1. The age distribution of the IIV4s and IIV3s vaccination groups in different gender was balanced (Supplementary Table S2). The seroconversion rates against H1N1, H3N2, B/Victoria, and B/Yamagata in the IIV4s-vaccinated subjects were 69.4% (50/72), 59.7% (43/72), 54.2% (39/72), and 51.4% (37/72), respectively. A total of 74 subjects were inoculated with IIV3s (40 male [54.1% (40/74)] and 34 females [45.9% (34/74)]. The seroconversion rates against H1N1, H3N2, and B/Victoria in the IIV3s vaccine recipients were 79.7% (59/74), 70.3% (52/74), and 36.5% (27/74), respectively. There was no statistical difference in the seroconversion rates against H1N1 and H3N2 between the IIV4s and IIV3s vaccine groups. However, the seroconversion rate against B/Victoria in the IIV4s vaccine group was higher than that in the IIV3s vaccine group (Table 1).
Item H1N1 H3N2 B/Victoria B/Yamagata IIV4s 69.4% (50/72) 59.7% (43/72) 54.2% (39/72) 51.4% (37/72) IIV3s 79.7% (59/74) 70.3% (52/74) 36.5% (27/74) −* χ2 2.04 1.786 4.605 −* p value 0.153 0.181 0.032 −* * Trivalent spilt vaccine do not contain B/Yamagata strain. Table 1. The overall positive rate of the IIV4s in Shenzhen and IIV3s in Changzhou, 2018–2019.
Among IIV4s-vaccinated subjects, 87.5% (63/72) had seroconversion against at least one of the influenza A strains, H1N1 and H3N2, among the IIV4s population at 30 days. Meanwhile, 68.1% (49/72) had seroconversion against at least one of the influenza B strains, B/Victoria and B/Yamagata, among the IIV4s population at 30 days. The highest seroconversion rates of all the four components were against H1N1 for both male [61.5% (16/26)] and female [73.9% (34/46)] subjects.
Different factors may impact the vaccine effects of the target components. There was a statistical difference between male and female subjects in the seroconversion rates against B/Victoria. The seroconversion rates against H1N1, H3N2, B/Victoria, and B/Yamagata were lower in the elderly group (≥60 years old; 24 [33.3%(24/72)] subjects) than in the adult group {18–59 years old; 48 [66.7%(48/72)] subjects}, and the rate ratios were statistically different (p<0.05). Health-care workers [29 (39.73%) subjects] had a significantly higher seroconversion rate against H3N2 compared with non-medical staff subjects (75.9% vs. 47.7%, respectively) (Table 2).
Characteristic IIV4s IIV3s H1N1 H3N2 B/Victoria B/Yamagata H1N1 H3N2 B/Victoria SR p SR p SR p SR p SR p SR p SR p Sex Male
(N=26)61.5%
(16/26)0.274 57.7%
(15/26)0.792 38.5%
(10/26)0.044 42.3%
(11/26)0.246 Male
(N=40)75.0%
(30/40)0.222 82.5%
(33/40)0.013 32.5%
(13/40)0.440 Female
(N=46)73.9%
(34/46)60.9%
(28/46)63.0%
(29/46)56.5%
(26/46)Female
(N=34)85.3%
(29/34)55.9%
(19/34)41.2%
(14/34)Age 18–59 years
(N=48)81.3%
(39/48)0.002 68.8%
(33/48)0.027 64.6%
(31/48)0.012 64.6%
(31/48)0.002 18–59 years
(N=48)83.3%
(40/48)0.295 66.7%
(32/48)0.357 43.8%
(21/48)0.078 ≥60 years
(N=24)45.8%
(11/24)41.2%
(10/24)33.3%
(8/24)25.0%
(6/24)≥60 years
(N=26)73.1%
(19/26)76.9%
(20/26)20.7%
(6/26)Healthcare workers Yes
(N=29)86.2%
(25/29)0.011 75.9%
(22/29)0.022 58.6%
(17/29)0.533 55.2%
(16/29)0.598 Yes
(N=21)76.2%
(16/21)0.634 61.9%
(13/21)0.592 33.3%
(7/21)0.723 No
(N=44)52.3%
(23/44)47.7%
(21/44)50.0%
(22/44)47.7%
(21/44)No
(N=53)81.1%
(43/53)73.6%
(39/53)37.3%
(20/53)Abreviation: SR=seroconversion rate. Table 2. Comparison of serum levels of seasonal influenza antibodies in Shenzhen and Changzhou between different groups, 2018–2019.
Among IIV3s-vaccinated subjects, 90.5% (67/74) had seroconversion against at least one of the influenza A strains, H1N1 or H3N2. In the IIV3s-vaccinated group, the highest seroconversion rates in male was against H3N2 (82.5%, 33/40) and H1N1 had the highest seroconversion rates among female subjects (85.3%, 29/34). In the adult group, the seroconversion rate against H1N1 was 83.3% (40/48), which is higher than that in the elderly group with the rate of 73.1% (19/26) (Table 2).
A multivariate analysis was performed on the 30-day seroconversion rates in the IIV4s- and IIV3s-vaccinated populations. An unconditional multi-factor logistic regression analysis revealed that, for the IIV4s-vaccinated group, the factors significantly influencing high seroconversion rates were age for H1N1, healthcare workers for H3N2, sex and age for B/Victoria, and age for B/Yamagata. In contrast, a similar analysis of the seroconversion rates at 30 days post-administration of the IIV3s vaccine group did not find any statistically significant factors (Table 3).
Item IIV4s H1N1 H3N2 B/Victoria B/Yamagata Affecting factors Age Healthcare workers Sex Age Age OR (95% CI) 5.515 (1.888, 16.109) 3.293 (1.164, 9.312) 0.358 (0.128, 1.004) 3.755 (1.305, 10.800) 5.775 (1.938, 17.208) p Value 0.002 0.025 0.037 0.014 0.002 Abreviation: OR=odds ratio; CI=confidence interval. Table 3. Binary logistic regression analysis of the IIV4s in Shenzhen, 2018–2019.
The changes in antibodies against seasonal influenza strains H1N1, H3N2, B/Victoria, or B/Yamagata in the surveillance subjects at different time points are followed up. For both the IIV4s and IIV3s influenza vaccination groups, the antibody level measured by geometric mean titer [GMT] at baseline (Day 0) was low (<20) in all subjects (Supplementary Table S3). In both the vaccine groups, the serum antibody GMT reached a peak at 30 days post-vaccination for all the components, after which the antibody titer gradually decreased with time. At 30 days post-vaccination, the GMT in IIV4s-vaccinated subjects against H1N1, H3N2, B/Victoria, and B/Yamagata were 91.37, 64.11, 35.64, and 40.00, respectively (Figure 1B). The antibody titers against H1N1 and B/Yamagata showed a downward trend from 30 days to 360-day post-vaccination, and the 360-day post-vaccination antibody titers decreased by 1.86 times and 1.4 times, respectively, compared with the 30-day HAI GMT titers. The control group showed a similar trend with low levels of the antibodies for all four time points. The serum GMTs against H1N1, H3N2, and B/Victoria from the IIV3s-vaccination subjects at 30 days post-vaccination were 147.06, 92.07, and 21.99, respectively (Figure 1C). The antibodies against H1N1 and H3N2 decreased significantly from 30 to 360 days post-vaccination.
Studies have demonstrated that a serum HAI GMT titer of ≥40 can prevent 50% of influenza infections (11). At 360 days post-vaccination, the percentages of IIV4s-vaccinated subjects with serum HAI titers against H1N1, H3N2, B/Victoria, and B/Yamagata of ≥40 were 60.6%(43/71), 52.1%(37/71), 39.4%(28/71), and 26.8%(19/71), respectively (Figure 1D); these percentages in the IIV3s-vaccinated subjects against H1N1, H3N2, and B/Victoria were 38.9%, 45.8%, and 69.4%, respectively (Figure 1E). In contrast, the percentages of IIV4s control group subjects with an HAI titer of ≥40 against H1N1, H3N2, B/Victoria, and B/Yamagata were 13.2%, 7.9%, 10.5%, and 5.3%, respectively; similarly, these percentages in the IIV3s control group subjects were 10.7%,7.1%, and 3.6% for H1N1, H3N2, and B/Victoria, respectively. Thus, the current influenza vaccine should be given not only before the current flu season, but also before the next flu season.
HTML
-
Different regions all over the world are annually affected by influenza. Thus, monitoring the serum antibody levels against the influenza vaccine can provide more scientific evidence for screening the effectiveness of influenza vaccine strains.
This study showed that the immunogenicity of IIV4s and IIV3s met the requirements for influenza vaccines, but IIV4s was immunologically superior versus IIV3s for the lineage B strain. The seroconversion rates of quadrivalent and trivalent split influenza vaccine are similar to those previously reported. Several studies have found that the individuals’ gender, age, health status, and immunization history may affect immune responses against seasonal influenza vaccine (12-13). In this study we found that age, gender, healthcare workers may affect seroconversion rates after vaccination. The observed seroconversion rates against H1N1 and H3N2 at 30 days post-vaccination in this study indicated that the immune effects of IIV4s vaccination is similar to that of IIV3s vaccination. However, we can notice that the positive seroconversion rate against B/Victoria among IIV4s-vaccinated group was higher than that in the IIV3s group. This better immune effect of the quadrivalent influenza (14) vaccine in the population may be due to the cross reactivity of the additional component B/Yamagata to B/Victoria. Meanwhile, this may be because of the geographic differences in the two cities we enrolled. Compared with the trivalent vaccine, the quadrivalent influenza vaccine has a wider scope of protection for the population, and the quadrivalent vaccine is especially beneficial when the B/Yamagata influenza virus is widespread.
The antibody levels peak at 30 days post-vaccination (15), and then decline so that considerable rates of the surveillance population will have insufficient HAI titers before the arrival of the next influenza season. Therefore, it will be necessary to receive another influenza vaccine before the next flu season arrives.
Based on the current influenza vaccine utilization, the vaccination effect varies between seasons. The timely surveillance of the vaccination effects will benefit strategic use of vaccines.
Acknowledgments: William J. Liu is a leading for this project. We thank all the participants and associated staff of Shenzhen CDC and Changzhou CDC for their help. Liumei Shu was responsible for the sample collection, testing, and data analysis of the project, and Jiezhang helped with the experimental work.
Funing: This work was supported by National Key Research and Development Program of China (grant 2017YFC1200202).
| Citation: |



 Download:
Download:




