-
The World Health Organization (WHO) released the World Report on Hearing on March 2, 2021. The WHO estimated that by 2050, nearly 2.5 billion (1 in 4 people) would be living with some degree of hearing loss, and at least 700 million of whom would require rehabilitation services (1). The risk factors that cause hearing loss not only include occupational but also non-occupational factors, such as, high-level exposure of noise and ototoxic chemicals at workplaces, age, excessive noise exposure in living environments or listening to loud music through personal listening devices, and ototoxic drug intake during childhood, etc. It was estimated that 16% of hearing loss might be contributed by exposure to high-levels of noise at the workplace (2). In occupational settings, high levels of noise are still the most focused issue all over the world. It was estimated that more than 30 million workers were exposed to hazardous noise in the United States of America (USA) (3). In Germany, 4–5 million people (12%–15% of the workforce) were exposed to noise levels defined as hazardous by the WHO (4). It is estimated that approximately 80 million workers in the total of 574 million workers in industrial and service settings in China are exposed to hazardous noise, and it is estimated that 14% of the workers in industrial and service settings in USA exposed to hazardous noise (5).
The exposure level for hearing loss in occupational setting was calculated as an A-weighted equivalent sound pressure level, averaged over the time of an 8-hours working day (LEX,8h), or 40 hours per working week (LEX,week) (3). The exposure limit of 85 dBA for occupational noise exposure recommended by the National Institute of Occupational Safety and Health (NIOSH) was reevaluated by incorporating the 4,000-Hz audiometric frequency into the definition of hearing impairment in the risk assessment (3). Current noise standards of hearing loss are based on the equal-energy hypothesis, especially for Gaussian (G) noise, e.g. ISO 1999:2013 (6), but not for complex noise. A statistic metric, kurtosis (β) had been developed for quantifying the complex temporal structure of a non-Gaussian (non-G) noise with measuring the peak (P), interval (I), and duration (D) histograms of the transients in the noise signal (7). Figure 1 showed the numbers of new cases of occupational noise-induced deafness diagnosed and reported from 2001 to 2019 in China. Although the numbers of new cases diagnosed and reported were dramatically increased after 2010, there is a huge gap between the numbers of cases diagnosed and the numbers of workers exposed to hazardous noise at workplace. The data from a cross-sectional survey with 6,557 workers of automotive industry showed that 28.8% of workers were found to have high-frequency noise-induced hearing loss (8). A meta-analysis with a total of 71,865 workers from transportation, mining, and typical manufacturing industries revealed that the prevalence of suspected occupational noise induced hearing loss in China was 21.3%, of which 30.2% was related to high-frequency noise-induced hearing loss, 9.0% was related to speech-frequency noise-induced hearing loss, and 5.8% was related to noise-induced deafness (9). In USA, a total of 15,900 new cases of recordable standard threshold shifts in 2017 that representing a rate of 1.4 cases per 10,000 workers were reported from the US Bureau of Labor Statistics annual Survey of Occupational Injuries and Illnesses (10).
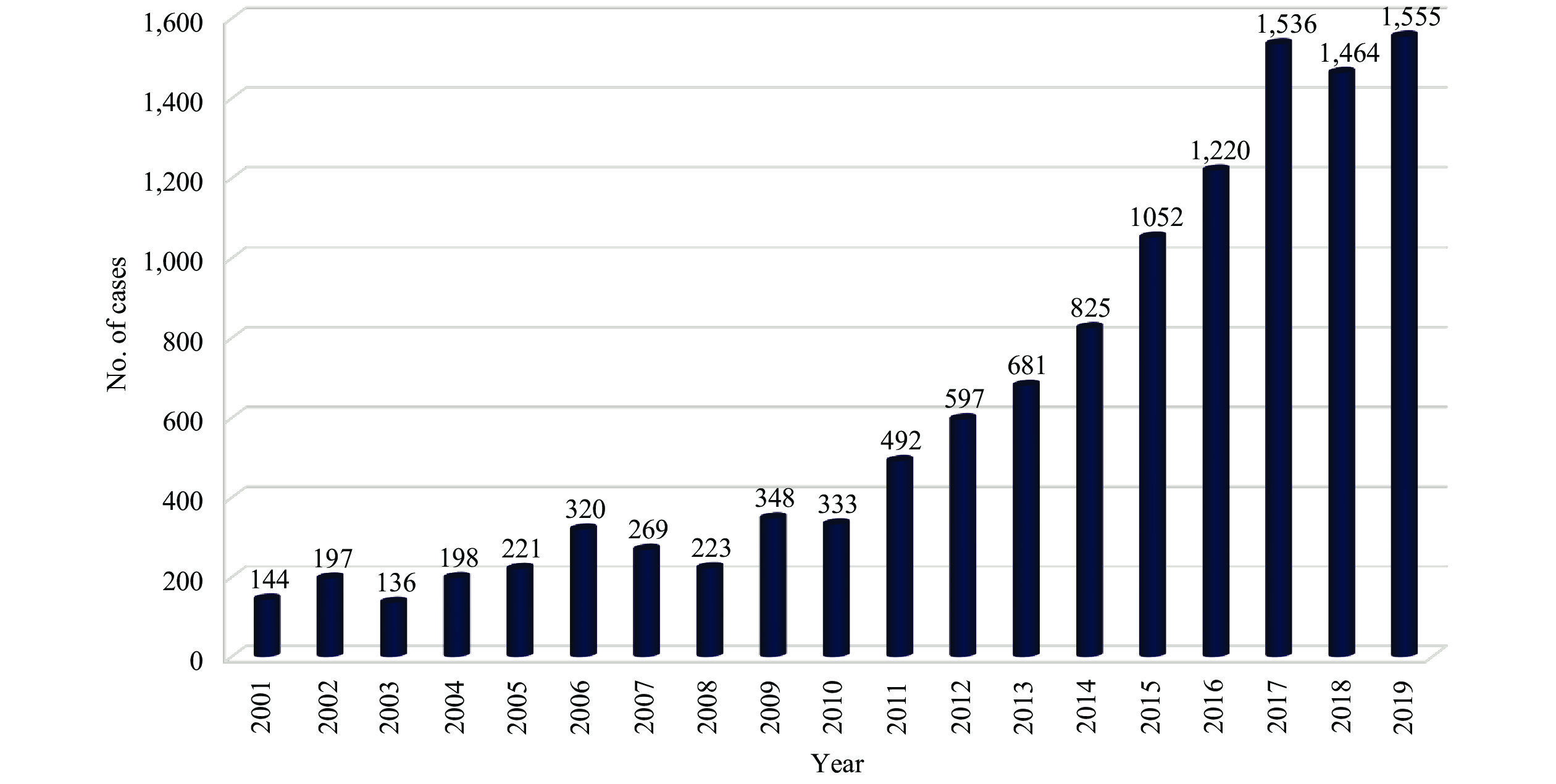 Figure 1.
Figure 1.Number of occupational noise induced deafness cases diagnosed and reported during 2001–2019 in China.
Note: Data from National Occupational Disease Report.Current studies found that noise exposure was not the only risk factor for hearing loss at the workplace as some chemicals used, either alone or in combination with noise or other chemicals, in industrial processes have been shown to have ototoxic effects (11). Current evidence demonstrates that some aromatic solvents have confirmed associations with exposure in the workplace and increased prevalence of hearing loss, including the following: toluene, styrene, ethylbenzene, p-xylene, methylstyrenes, allylbenzene, and n-propylbenzene; some non-aromatic solvent such as trichloroethylene, nitrile, and asphyxiants; and some metals or its compounds such as lead or its compounds (11). Our research investigated the hearing loss of workers by combined exposure of ototoxic organic solvents and noise in wood furniture manufacturing factories and printing factories. The results of our study indicated that hearing loss of workers caused by combined exposure of organic solvents and noise was serious as high frequency hearing loss and speech frequency hearing loss were affected. Noise is a physical factor that causes mostly mechanical and metabolic damage to the peripheral auditory receptor, cochlea, and the auditory neural pathways (12-14). Ototoxic chemicals in the bloodstream go through either the blood-labyrinth barrier into the cochlea or the blood–brain barrier to the eighth cranial nerve and central nervous system (14-15). As a result, chemical-induced hearing loss can result from the effects on several sites in the hearing system. Ototoxic chemicals may affect the structures and/or the function of the inner ear (auditory and vestibular apparatus) and the connected neural pathways.
The workers exposed to hazardous noise may experience multiple adverse health outcomes, including communication difficulties, social isolation, stress, and fatigue (16), and these adverse health outcomes are probably associated with depression, cognitive decline, dementia, fall, increased hospitalization, and health care costs (17-18). High levels of noise are associated with tinnitus, hyperacusis, cardiovascular disease, annoyance, performance decreases, and sleep disturbances (16-18). High levels of noise exposure during pregnancy may be associated with adverse reproductive outcomes, including low birthweight and preterm birth (19). In China, the huge numbers of workers exposed to hazardous noise will increase the burdens in diagnosis and economic costs of disease. The best approach is to improve a comprehensive strategy to control and reduce the exposure level of noise in workplaces and improve health promotion of workers.
We are currently establishing a prospective cohort to investigate the impact on workers of hearing loss and related adverse outcomes due to exposure of noise and combined exposure to noise and ototoxic chemicals at workplace. Data from this ongoing study will provide evidence for better understanding of health impacts and mechanisms of hearing loss and related diseases and for revision of occupational health and occupational diagnosis standards, e.g. occupational exposure limits for noise in the workplace and the diagnosis of occupational noise-induced deafness.
HTML
| Citation: |





 Download:
Download:




